Introduction
Material and Methods
Searching articles and evolution
Result Analysis
Discussion
Machine learning and deep learning in clinical diseases
ML and DL in human resource management
Conclusions and Recommendations
Introduction
Sustainable urban development depends fundamentally on resilient health systems and healthy populations. Within the Sustainable Development Goals, ensuring good health and well‑being (SDG 3) underpins inclusive, productive, and equitable cities (SDG 11). Urban healthcare organizations therefore carry a dual mandate: protect occupant health through timely prevention, detection, and intervention, and sustain a capable of workforce that can adapt to shocks and long‑term demographic pressures [1]. Yet many providers face mounting clinical complexity, fluctuating demand, and persistent human‑resource constraints that complicate decision‑making and strain operational capacity [2, 3, 4].
Artificial intelligence particularly machine learning (ML) and deep learning (DL) has emerged as a practical means to transform heterogeneous clinical and operational data into actionable insight, supporting earlier diagnosis, targeted interventions, and smarter workforce planning. Global bodies such as the World Health Organization recognize the potential of digital health while emphasizing that technology should augment—not replace—clinical judgement and established models of care, with careful attention to benefits, risks, feasibility, and equity [5].
ML/DL techniques are now embedded across key healthcare tasks. In clinical decision support, supervised models and ensemble methods predict and stratify disease risk for conditions such as nephrolithiasis, diabetes, coronary heart disease, and cancers, enabling more precise triage and follow‑up [6, 7, 8, 9, 10, 11, 12, 13]. Data quality remains a limiting factor; to address sparse or imbalanced datasets, DL‑based augmentation (e.g., generative adversarial networks) and multimodal fusion improve medical image quality and downstream classification, advancing tumor and lesion detection [14, 15, 16, 17]. Emerging large language models show promise as assistive tools for clinicians, streamlining information retrieval and documentation while requiring rigorous evaluation and governance [16].
On the operational side, ML/DL contributes to sustainable workforce planning by forecasting demand, optimizing staffing and scheduling, reducing wait times, and mitigating burnout risk. Predictive models for turnover, length of stay, and recruitment outcomes help align skills with need and reduce costly attrition, while speech and workflow analytics can lower administrative burden and enhance team performance [18, 19, 20, 21, 22]. Together, these advances support the dual sustainability goals of better health outcomes and a stable, efficient healthcare workforce in urban settings.
Despite rapid progress, important gaps persist: fragmented and non‑standardized datasets, variable external validity across institutions and populations, bias and fairness concerns, privacy and interoperability barriers, and limited reproducibility of reported results. Clear reporting standards, robust validation, and human‑in‑the‑loop deployment are needed to translate performance gains into durable improvements in care and workforce resilience.
In this context, the present work provides a PRISMA‑ guided systematic review focused on healthcare applications most relevant to sustainable urban development: occupant health (surveillance, risk prediction, diagnosis, and care‑pathway support) and workforce planning (demand forecasting, staffing, scheduling, and retention). We map tasks to methods (tree‑based learners, CNN/RNN/LSTM architectures, transformers, generative models), summarize data sources (EHRs, imaging, wearables and ambient sensors, administrative records), assess evaluation practices, and identify research and implementation gaps. Our goal is to offer a clear, evidence‑based synthesis and a practical roadmap for leveraging ML/DL to strengthen urban health systems while safeguarding quality, equity, and clinician oversight.
Material and Methods
Searching articles and evolution
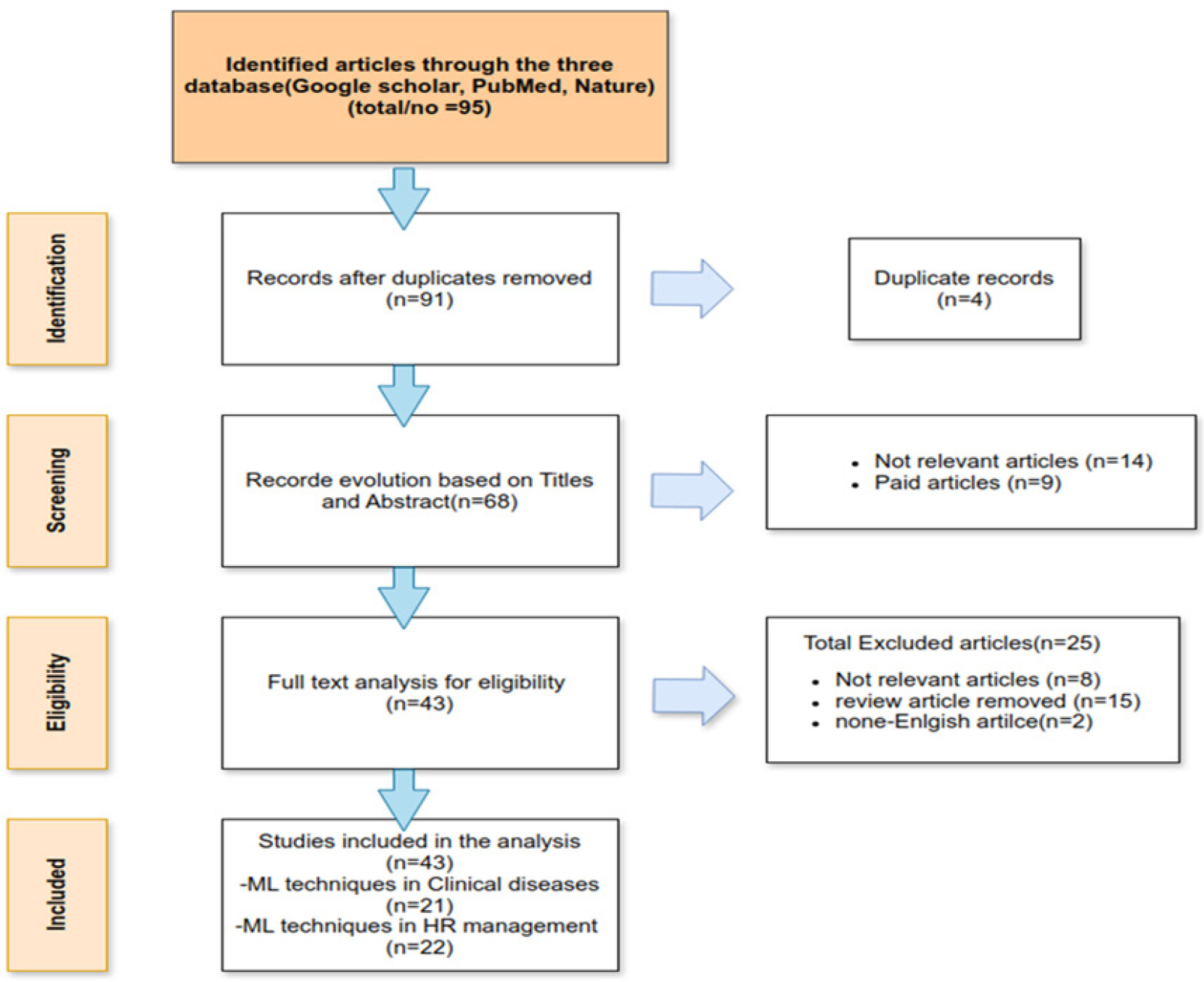
We collected articles from three databases (Pub Med, Google Scholar, and Nature Porfilio). These articles were filtered between January 1, 2019, and May 30, 2025, based on titles and abstracts using keywords and Boolean operators such as “machine learning techniques” OR “deep learning methods” AND “clinical disease” OR “human resources management” AND “healthcare organization”. Additionally, we applied a snowballing strategy to avoid missing relevant articles. After collecting relevant studies, we followed the PRISMA statement [23]. Figure 1 demonstrated the overview of selecting and evolution of articles.
Result Analysis
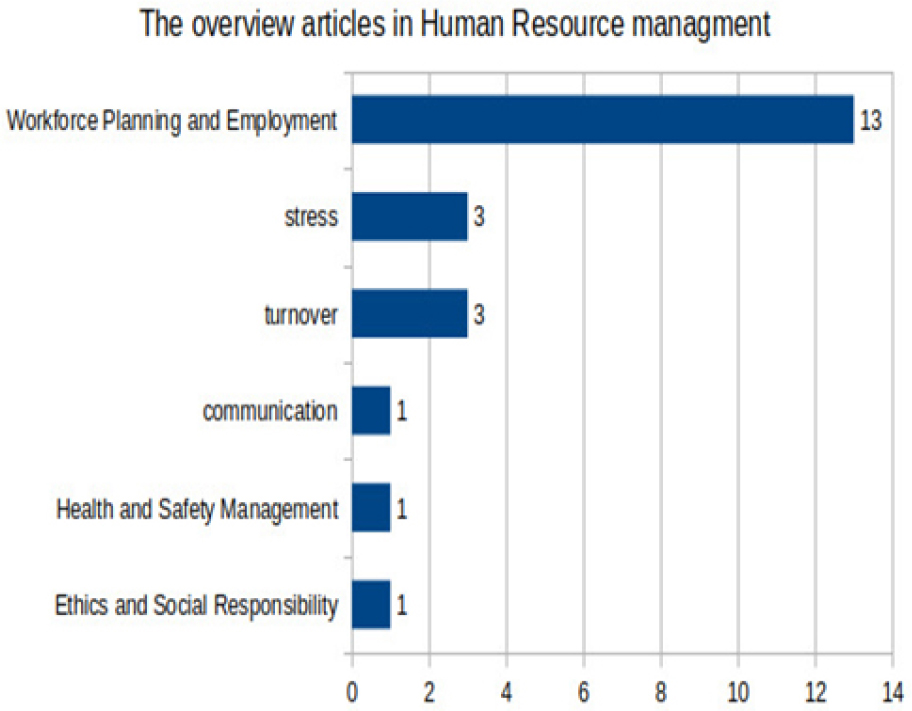
We collected 95 articles after applying search strategy, then The titles and abstracts of the search results were screened independently by all authors. Then we obtained 68 articles after removing duplicate records and paid articles. In the next stage, 43 articles selected after the remaining records were analyzed using the full-text versions and removing irrelevant articles including, non-English studies, and omitting review articles. Finally, we selected 43 articles in which 21 mainly focused on clinical diseases. 9 papers discussed the implementation of various ML and DL methods in order to anticipating COVID-19 infection in patients from clinical disease articles. Table 1 presents detailed information on several research studies that have been applied for the early identification of COVID-19. The remaining 12 articles primarily addressed various clinical conditions, including, cancer [24], liver disease [25, 26], complex chronic pain [27, 28], heart diseases [29, 30, 31], risk of delirium [32], HIV [33], eyes diseases [34] and human emotion detection [35, 36, 37, 38, 39, 40]. Among the 43 articles reviewed, 22 pertain to human resource management as illustrated in Table 2 and Figure 2. These articles mostly discussed regarding to improve workforce planning employment due to different challenges in human resource management sectors in healthcare organization.
Table 1.
Overview of ML and DL for identifying COVID-19
| Ref | Objective (Tasks) | Methods | Data source | Contribution |
| Muhammad Imad et al. [41] | Detection of COVID-19. | SVM, KNN, RF, DT and Naïve Bayes | Kaggle repository (Kaggle, 2020) | The study provides significant method to classify COVID-19 infected patients. the results show support vector machine obtained the highest accuracy 96%. |
| Pınar CİHAN et al. [42] | Forecasting the number of serious care case, intubated patients and deaths. |
RF, Bagging, KNN Support Vector Regression (SVR), Classification and Regression Tree | Ministry of Health of Turkey (between 27 March 2020, and 28 July 2020) | this work presented remarkable results and The RF model provided the highest prediction for the number of intensive cases of COVID-19. |
| Bradley S. Price et al. [43] | forecasting the expected increase in COVID-19 cases in the short term. |
Rt Only Method, ML+Rt Method: Long Short-Term Memory (LSTM) | WV Department of Health 87 and Human Resources (WVDHHR). | The study discussed new approach and applied two methods for 55 counties in the state of West Virginia. |
| Shanbehzadeh et al. [44] | predicting re- hospitalization risk of covid-19 patients | DT, SVM, KNN, hybrid algorithm (named Water wave optimization) | academic hospital in Abadan, Iran | The Water wave optimization model obtained the significant results compared to other models in order to forecasting readmission risk COVID-19 patients. |
| Varzaneh, Z. A et al. [45] | forecasting covid-19 classification | Features selection, DT, SVM, Multi-Layer Perceptron (MLP), KNN | Imam Khomeini hospital, Ilam city, Iran | The study achieved strong results for estimating the necessary of intubation in COVID-19 cases utilizing machine learning and meta-heuristic feature selection techniques. |
|
Kolluri N et al. [46] | Forecasting Misinformation Counteraction of COVID-19. | Bidirectional Long Short-Term Memory (Bi-LSTM), SVM, Logistic Regression (LR), Bernoulli Naive Bayes (BNB), BERT, XLNet, Convolutional Neural Network (CNN) | CoAID, Fake News Net (FNN), Politi Fact, Gossip Cop, Poynter, News API, | proposed an automated model for anticipating inaccurate information utilizing machine learning technique. |
|
Yazdani A et al. [47] | COVID-19 prediction using machine learning | SVM, Naive Bayes, LR, RF, K-NN algorithms | Shiraz University, Iran | The results indicated that SVM model with 93.41% accuracy achieved the highest performance for classification. |
| Abugabah A et al. [48] | multi-day prediction of covid 19 |
Gated-Recurrent Unit, Long Short-Term Memory (LSTM). linear regression, Auto-regressive moving average (ARIMA) | Algerian ministry of the health from 25 February to 12 November 2020 | the proposed model has employed a comprehensive comparison of the Gated-Recurrent model represented outperformed then other prediction methods for understanding the early notices and control the pandemic. |
|
Yazdani A et al. [49] | forecasting the recovery rate of hospitalization of COVID-19 patients using machine learning techniques. | KNN, RF, decision tree (DT), Naive Bayes (NB), multilayer perceptron (MLP) | Valiasr Hospital, Iran | The experiments of study indicates that NB algorithm has better performance compare to other machine learning for anticipating of survival covid-19 patients. |
Table 2.
ML and DL Techniques in Human Resource Management
| Authors | Methods | Area | Contribution |
|
Patel, D et al. [50] | Bio-clinical BERT, Bag-of-Words Logistic Regression with TF-IDF features (BOW-LR-tf-idf). | Workforce Planning and Employment | The study indicate to the growing body of literature in the field of natural language processing and machine learning in healthcare. |
|
Ahmad Hamdan, A. F et al. [51] | LR, DT, k-NN, Naïve Bayes (NB), RF, Gradient Boosting (GB), Multilayer Perceptron (MLP) | Workforce Planning and Employment | The study contributes by developing a machine learning-based predictive model for outpatient no-show appointments, achieving the highest performance with a Gradient Boosting algorithm and providing insights for interventions to reduce no-shows. |
|
Mattie, H et al. [52] | RF, LR | Workforce Planning and Employment | Impact ability of healthcare interventions using machine learning, administrative claims, sociodemographic, and patient-generated data to optimize resource allocation and improve health outcomes. |
| Aufegger, L et al. [53] | LR, DT, k-NN, Naïve Bayes (NB), RF, Gradient Boosting (GB), Multilayer Perceptron (MLP) | Workforce Planning and Employment | The study contributes by developing a machine learning-based predictive model for outpatient no-show appointments, achieving the highest performance with a Gradient Boosting algorithm and providing insights for interventions to reduce no-shows. |
|
Triberti, S et al. [54] | AI discussed | Stress management | integration of AI in healthcare decision-making, including delayed decisions, miscommunication, and role ambiguity between patients, doctors, and AI systems. |
|
Sandhu, S et al. [55] | Multi-Output Gaussian Process Recurrent Neural Network (RNN), | Workforce Planning and Employment | The article contributes by examining the factors influencing the integration of a machine learning-based sepsis early warning system into clinical workflows, highlighting themes such as trust, workforce considerations, and strategies to improve adoption and clinician engagement. |
|
Kumar, P et al. [56] | - | Ethics and Social Responsibility | establishing a framework for “Responsible AI” in healthcare as a third-order formative construct that demonstrates its influence on patient cognitive engagement and perceived value creation. |
|
Yang, Y et al. [57] | Cascaded Deep Learning Model, Recurrent Neural Networks (RNNs), Restricted Boltzmann Machines (RBMs), RNN-RBM Deep Neural Network Model | Workforce Planning and Employment | The study provides by developing and validating a cascaded deep learning and probabilistic mining model to analyze healthcare big data, predict hospital outpatient volumes, and optimize medical resource allocation. |
|
Yakusheva, O et al. [58] | Random Forests | Workforce Planning and Employment | uncovering a nonlinear U-shaped association between nurse staffing and 30-day hospital readmissions using machine learning, identifying tipping points where additional nurse staffing no longer improves and may worsen readmission outcomes. |
|
Cuadrado, D et al. [59] | Random Forest, XGBoost, LightGBM | Workforce Planning and Employment | proposing a hybrid machine learning model that combines length of stay and days to discharge predictions, improving ICU discharge date estimations with reduced prediction errors, and enabling better resource planning and patient management. |
|
Arias, J. C et al. [60] | SVM, Generalized Linear Models (GLM) | Workforce Planning and Employment | developing predictive models using machine learning to estimate emergency healthcare demands for respiratory diseases, enabling efficient resource allocation and response planning. |
| Lai, CH et al. [61] | LightGBM, XGBoost Algorithm, CatBoost, Artificial Neural Networks (ANN), Google’s Wide & Deep Learning | Workforce Planning and Employment | developing machine learning models to predict the length of hospital stay in geriatric fragility fracture patients, demonstrating the potential of AI techniques to optimize healthcare resource allocation and improve patient outcomes. |
| Yang, Y et al. [62] | LR, RF, XGBoost | Workforce Planning and Employment | The article develops and evaluates machine learning models to predict the likelihood of missed appointments in healthcare, leveraging administrative data to optimize resource allocation and improve health equity. |
| Liu, L et al. [63] | Naïve Bayes Classifier, LR, SVM, Decision Tree, RF, Gradient Boosted Logistic Regression (GBL), Artificial Neural Networks (ANNs), Deep Learning Algorithm using TensorFlow | Workforce Planning and Employment | developing and evaluating machine learning models to predict last-minute pediatric surgery cancellations based on patient-specific and contextual data, identifying key predictors, and demonstrating the potential for targeted interventions to reduce healthcare costs and improve patient and family experiences. |
| Tsai, J et al. [64] | YOLOv3, Deep SORT, FaceNet Inflated 3D ConvNet (I3D), Non-Maximum Suppression (NMS), | Health and Safety Management | This paper contributes to intelligent surveillance by proposing a real-time deep learning-based system for detecting multi-person actions, making it particularly suitable for environments such as long-term care facilities. |
| Zhang, X [65] | ARIMA model, Simple Exponential Smoothing (SES) model | Workforce Planning and Employment | This paper proposes and validates a hybrid ARIMA and SES model to predict daily visits to the outpatient blood sampling room with improved accuracy, which helps in optimal resource allocation and management in hospitals. |
| Devyania, R. D [66] | General impact of AI | Workforce Planning and Employment | This document shows how AI has transformed human resource management in China’s healthcare industry during the COVID-19 pandemic by improving recruitment, training, performance, and operational efficiency. |
| Lieslehto, J [67] | SVM, K-NN | Stress management | This study shows that machine learning models can predict healthcare workers’ psychological resilience and likelihood of sickness absence, enabling early individualized diagnosis and targeted interventions to support mental health. |
| Zhang, Y [68] | Artificial Neural Networks (ANNs), Convolutional Neural Networks (CNNs), Recurrent Neural Networks (RNNs), Long Short-Term Memory (LSTM) Networks | Stress management | This study contributes to the development and validation of a deep learning-based approach to predict worker stress levels using classification and regression models, demonstrating its potential for improving human resource management in companies. |
| Meddeb, E [69] | Graph Representation Learning, | Turnover | This paper contributes by proposing a predictive model that combines machine learning and system dynamics algorithms to predict employee turnover rates. |
| Pourkhodabakhsh, N [70] | LR, Decision Tree, RF, SVM, Gradient Boosting, AdaBoost | Turnover | This study helps provide a decision support tool for managers to effectively predict and reduce turnover rates by proposing a combination of meta-heuristic algorithms, feature selection methods, and multi-criteria decision-making techniques to identify and evaluate factors affecting employee turnover. |
| Zhu, H [71] | Backpropagation Neural Networks (BPNNs), Gradient Descent Optimization Algorithms | Turnover | This paper proposes innovative machine learning-based algorithms to enhance human resource management systems by improving the accuracy of salary forecasting, employee turnover prediction, and human resource allocation. |
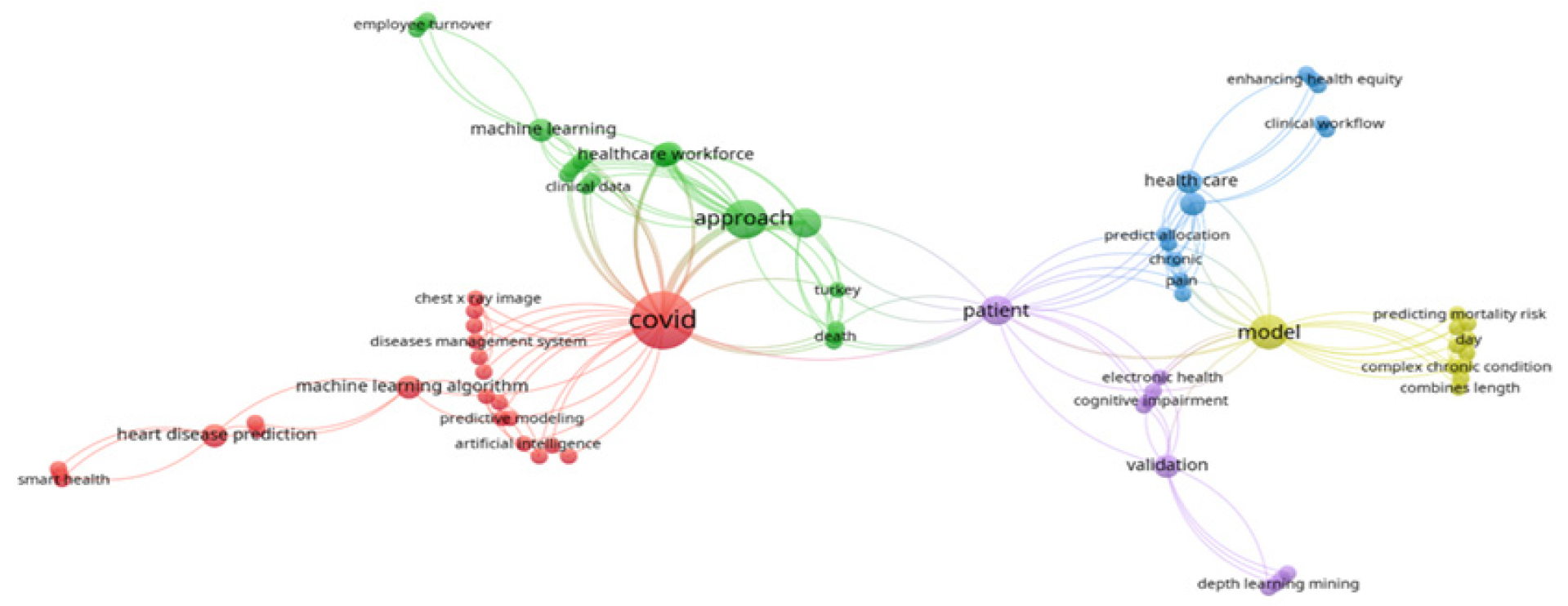
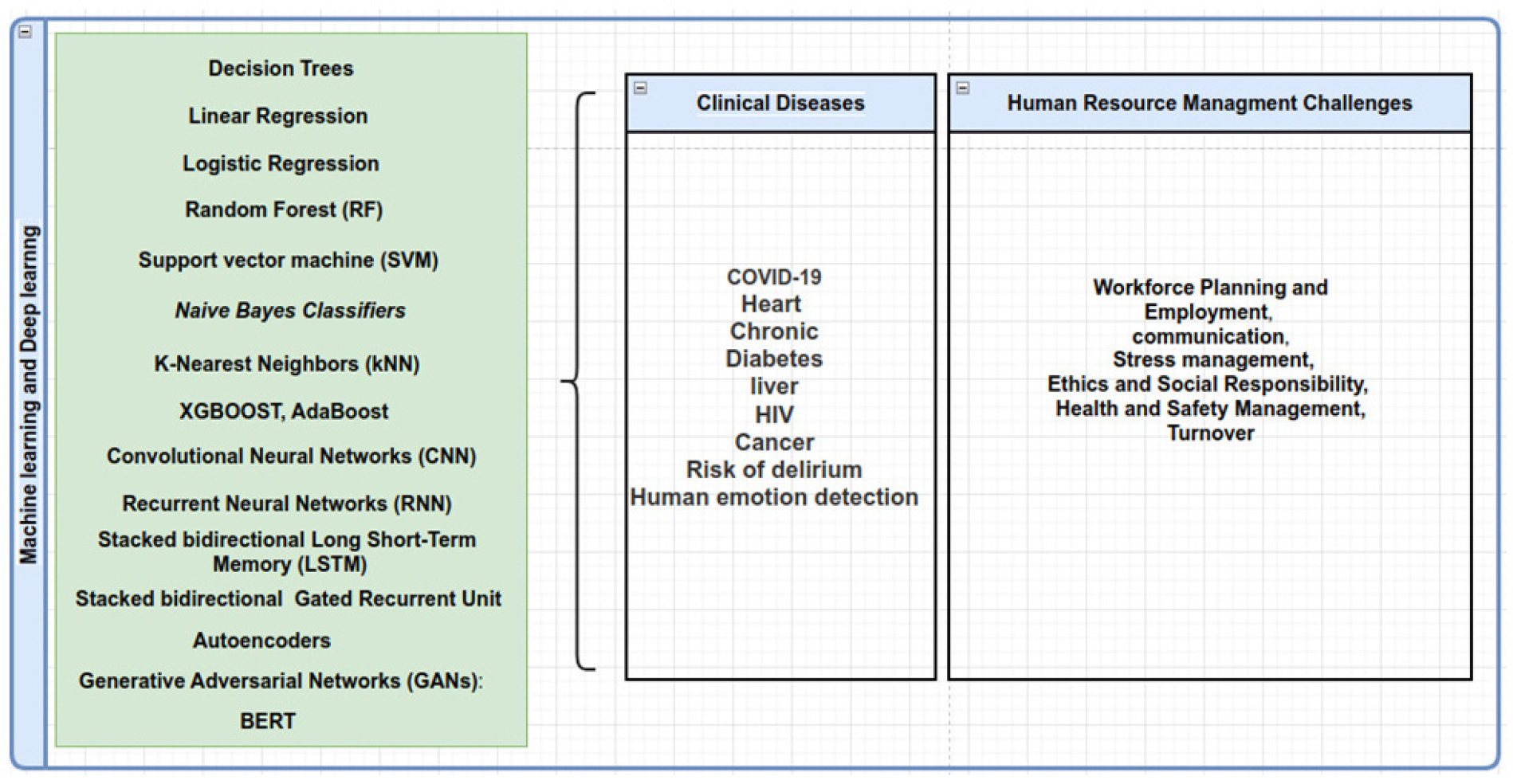
Our findings show that the Support Vector Machine (SVM), Logistic Regression (LR), Decision Tree (DT), Gradient Boosting, Neural network, Random Forest (RF), XGBoost, K-Nearest Neighbor (KNN), Long Short-Term Memory (LSTM) neural network, Recurrent Neural Networks (RNN), Convolutional Neural Net works (CNN), AdaBoost, and Naïve Bayes (NB) have been mostly used to deal with clinical disease and human resource management in healthcare organization. Figure 3 shows an overview of the detailed information about the most common machine learning and deep learning methods in clinical disease and human resource management within the healthcare organization. We also obtained the most occurrence of top keywords addressed by machine learning in clinical disease and human resource management using VOSviewer software [36]. Figure 4 demonstrated the most top keywords regarding to clinical diseases and human resource addressed by machine learning.
Discussion
Machine learning and deep learning in clinical diseases
Machine learning and deep learning can have significant impact on different level of clinical experiments and investigation that can make contribution to achieve targets for ameliorate personalization and more effective healthcare organization [37]. Machine learning and deep learning techniques can accelerate the process of analysing clinical data to effectively identify crucial details of patients for various disease identification [38]. To achieve accurate predictions, both supervised and unsupervised algorithms are utilized. these methods have rapidly implemented in healthcare sector to provide more efficient diagnosis solutions in order to deal with classification problems and predicting the symptoms of early diseases [39, 40].
Machine learning models can use to forecasting several diseases such as complex chronic conditions [27, 28], liver disease [25, 26], eye diseases [34], human emotion recognition [35], HIV infection [33], risk of delirium [32] as well as to perform tasks like as heart disease [29, 30, 31]. Guillamet et al. proposed a machine learning model which mainly focus on mortality risk in patients with complex chronic conditions. the study can show the important points of each case of risk of mortality using graphs which can make contribute to efficiently identify cases in which need more attention care by health care providers [27]. The study [28] demonstrated six questionnaires with five machine learning algorithms in order to figure out chronic pain in patients. The research indicates that the Neural Network and XGBoost algorithms figure out the best accuracy in prediction. The study can reduce the cost and improve the chronic pain management. Mounita Ghosh et al. conducted a comprehensive study for liver disease prediction using machine learning and the result shows that random forest algorithm obtained the best performance for liver disease prediction with highest accuracy compare to K-Nearest Neighbors, LR, SVM, DT, Extreme Gradient Boosting, AdaBoost [26]. Generative artificial intelligence is a robust algorithm designed to generate text, audio, and images. it has been rapidly incorporated into medical science to solve complex medical problems recently [72].
GAN systems are able to improve the speed of healthcare delivery and reduce costs. [73]. For example, it can capture the conversation between the doctor and patients and note it. recent research shows that these tools are useful to improve the management in healthcare [74].
Yuki Sahashi et al. developed a deep learning model called EchoNet-Liver. The model is able to find signs of liver disease using heart ultrasound videos, which contributes to early detection of chronic liver disease. They applied convolutional neural network for video classification and quality control and DenseNet used for disease detection, DenseNet model was trained using binary cross-entropy loss, Adam optimizer used for minimizing the binary cross-entropy loss during the training model for liver diseases detection form echocardiography images. The authors conclude this could enable cost-effective, opportunistic screening during routine echocardiograms, through the retrospective design and preprint status are important limitation [75].
Conversely, Levy et al. demonstrated a deep learning model to use Generative Adversarial Networks (GANs) to convert H&E-stained images into trichrome stained images in order to predict non-alcoholic steatohepatitis liver disease. the proposed model significantly reduces the cost and time in which shows the effectiveness of the technology. furthermore, could be implement into the clinical workflow as a diagnostic aid [25].
One of the important eye diseases is Age-related macular degeneration (AMD), by applying computer- aided frameworks, the researchers exhibited early identification of the condition of eye diseases in order to identify timely intervention and adaption to personal cares. the proposed model applied server traditional machine learning methods for classification and optimization in order to obtain outstanding results. they employed various metrics performance such as accuracy, sensitivity, specificity, ROC, F1-score and balanced accuracy [34]. ASHA. P et al. conducted a study to human emotion recognition in a low resource environment using machine learning algorithm. the study employed support vector machine for classification of six human emotion feeling such as fear, disgust, sadness, happiness, surprise, and neutral in order to optimize of memory and processing limitation [35]. The other study investigated on prediction of risk of delirium without account cognitive impairment. The study found that the gradient boosting algorithm obtained better result compare to penalized logistic regression and random forest algorithms [32]. Allan Kimaina et al. have applied several statical machine learning methods using electronic health record data in order to predict the viral failure. the study demonstrated the significance of early identification of viral failure utilizing a large HIV care program in Kenya which can apply the necessary interventions in advance. The approach determined that ensemble techniques such as support vector machine. gradient boosting machine (GBM), XGBoost and Bert achieved the best model’s performance and accuracy in order to predict viral failure [33]. The other study discussed heart disease prediction by applying K-NN, DT, RF, SVM and Naïve Bayes (NB). the result shows that ReliefF + SVM and RFS+ SVM, achieved better classification performances compared to other combined model classifiers [29]. Similarly, Zeinab Noroozi et al. demonstrated the key role of feature selection methods in improving model performance for predicting heart diseases. The study provided a detailed comparison of different feature selection algorithms and machine learning models for heart disease prediction. Ten-fold cross-validation was used to evaluate the models. the research contributes to health decision-makers, clinical experts, and researchers by enabling them to employ new technologies in forecasting heart disease [30]. Moreover, Shawni Dutta et al. developed deep learning models for heart disease prediction. They examined Stacked Bidirectional Long Short-Term Memory (LSTM) and Stacked Bidirectional Gated Recurrent Unit [31]. that shows these techniques able to deal with complex problems effectively.
ML and DL in human resource management
The first generation of human resource management was introduced in the 1960s, which mainly focused on designing automatic systems for calculating employee data [76]. As artificial intelligence technology progresses, machine learning, deep learning methods, and human resource management strive to improve data sharing and manage risks to obtain innovative and more optimized solutions in organizational systems, especially in healthcare organizations [77]. The human resource management in organizational systems strives to tackle challenges such as data privacy [78], hospitalization [79], communication [53], turnover [69, 70, 71], stress [54,67,68], and forecasting health care demands in urgent situation [60]. In the realm of healthcare, hospitalization is a crucial challenge in hospitals [79], wherein several factors contribute to it, including administration, managing patients, readmission, and ensuring efficacious resource allocation. Moreover, There are several research to explore the beneficial of machine learning algorithms regarding to predicting hospitalization [79], Long-term Length of Stay and days to discharge, admission, cancelling the appointments, [59,61, 62, 63], by utilizing naïve Bayes, support vector machine (SVM), decision trees, random forests (RF), light gradient boosted, XGBoost, CatBoost and Artificial Neural Network (ANN), Incorporating machine learning methods with traditional methods is an effective solution to achieve organizational objectives.
It is also paramount to have effective Health and Safety Management in healthcare organizations. These environments deal with challenges such as patient- employee interactions, teamwork and management among healthcare professionals, and the need to reduce costs and time. to tackle the issues, several studies have been investigated in order to enhance the quality of performances in healthcare organizations using machine learning and deep learning algorithms including Recurrent Neural Networks (RNNs) and Restricted Boltzmann Machines (RBMs), YOLO (You Only Look Once), Deep SORT, FaceNet and Inflated 3D ConvNet (I3D) [62, 64].
Predicting employee turnover is a critical indicator for a company’s health [71, 80]. Consequently, it could be a source of frustration and displeasure with work situations, as well as ineffective management. on the other hand, machine learning methods can providing significant solutions for improving the performance activities and better human resource management. the author focused on extracting useful features for predicting turnover based on onion model, in order to analysis the effectiveness of various retention strategies using machine learning techniques [69]. Moreover, the other research discussed the identifying the key factors that cause employee turnover by utilizing various algorithms, including Mutual Information, Recursive Feature Elimination algorithm, Meta-heuristic algorithms such as Gray Wolf Optimizer and Genetic Algorithm, and Multi-Criteria Decision-Making techniques. They employed the IBM dataset, which contains 1470 employees and 38 features. The following ML techniques have been applied to identify the key factors of employee turnover: DT, LR, RF, SVM, Gradient Boosting, and Adaptive Boosting. The results provided valuable information for recognition of the key factors affecting employee turnover using the Mutual Information algorithm [70].
Stress is known as “a condition of mental strain or pressure due to upsetting conditions” [81]. Stress is a critical problem in modern healthcare, which can have a negative impact on dealing with challenges. it’s required to control the stress to reduce the employee’s mental problems. Machine learning and deep learning can be used as effective tools for early detection of employee stress to have an effective plan in order to reduce workload and create a pleasant workplace environment [82]. A study demonstrated that managing stress is a thoughtful task for the human resource management (HRM) department using deep learning techniques to enhance management in the healthcare system. The authors claimed that stress has negative effects on employees’ performance in the workplace. They suggested an effective deep learning model to estimate and identify the workers’ stress levels with its key factors such as salary, working time. They concluded significant results with 71% accuracy for the classification model, which can make a contribution to improving the human resource management in enterprise companies [68]. Thus, Machine learning and deep learning are effective tools for identifying stress factors such as salary or working hours, which can help healthcare organizations. Data privacy is a pivotal factor in healthcare organizations [78], and it is necessary to protect patient information. A comprehensive study presented the effect of understanding the responsibility of artificial intelligence to analyse and identify its key factors in value formation and market performance in the healthcare system. They applied artificial intelligence in various domains in healthcare, and their findings show that AI technologies can replace traditional methods for improving healthcare performance. In addition, they discussed the main challenges, including data privacy, security, and equitable distribution of benefits [56]. Healthcare organizations play an important role in the service sector of any society [83]. Hospitals are important sectors that deal with emergency cases and should have better intensive care units to treat patients. A study investigated forecasting health care demands in urgent situations and helped to prepare effective plans to enhance the performance of human resources [60]. As we have highlighted, artificial intelligence methods play an outstanding role in addressing various challenges in human resource management to enhance performance quality, thereby helping healthcare organizations achieve their objective.
Limitation
Although machine learning and deep learning hold significant promise in sectors such as healthcare, several challenges remain in implementing these technologies effectively.
Data Quality and Privacy
Since datasets are an important aspect for training any machine learning model, protecting patient data is a vital task; moreover, data collected from diverse sources can sometimes be of low quality, which can lead to the development of weak models [84].
Time-Consuming Tasks
The integration and deployment of AI technologies to solve real-time problems are extensive and time- consuming tasks; therefore, we still have a long way to go in optimizing these processes [85].
Lack of Expert Personnel
Incorporating new AI technologies with existing clinical disease management and human resource methods requires specialist personnel; however, the lack of experts in this interdisciplinary field poses significant challenges [86].
Prediction and Accuracy
While machine learning and deep learning models provide outstanding innovative solutions in the healthcare sector, there are still problems with the accuracy of predictions in classification problems, necessitating further work to improve them [87].
Conclusions and Recommendations
Machine Learning (ML) and Deep Learning (DL) have demonstrated remarkable potential in advancing sustainable healthcare infrastructure and facility management. These technologies aid in early detection of diseases such as COVID-19, cancer, diabetes, and liver or skin disorders, thereby reducing the burden on healthcare systems and improving patient outcomes. Beyond clinical diagnosis, ML and DL enhance human resource management in hospitals by optimizing communication, reducing stress, and supporting emergency healthcare services. Such improvements directly contribute to sustainable building operations, as efficient healthcare delivery relies on robust facility management, resource allocation, and integration of smart technologies. However, challenges remain in embedding AI seamlessly within clinical workflows, often requiring specialized expertise and extended implementation time. This study highlights how incorporating AI with traditional methods can enhance healthcare facility sustainability, resilience, and service quality—offering critical insights for sustainable building design, management, and policy within urban development contexts.